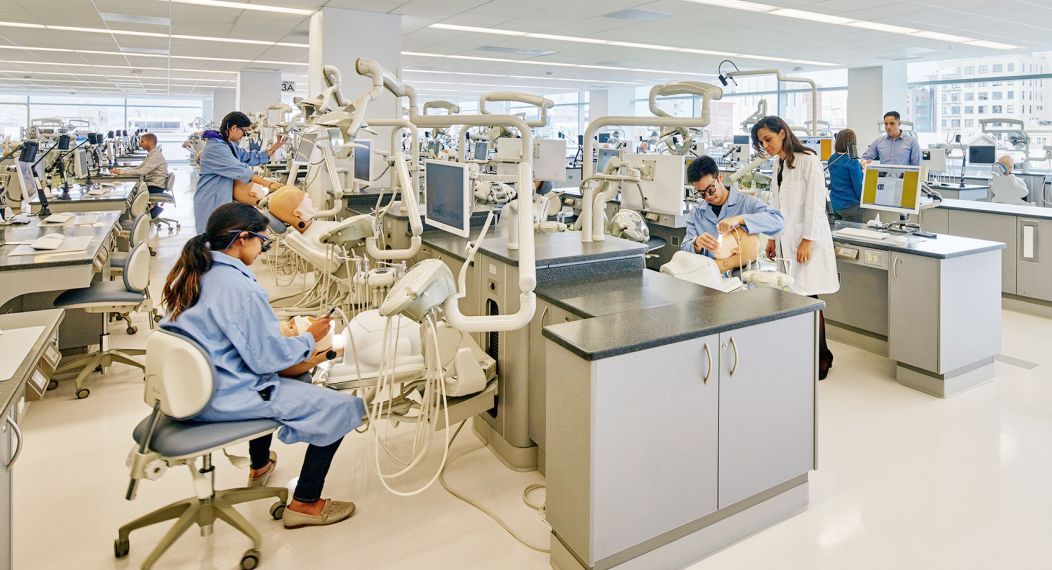
The Pacific Oral & Maxillofacial Pathology Laboratory is a private practice with three board-certified oral pathologists. We process and diagnose tissue samples 24 hours after receipt. All reports of malignancies and serious disorders are given over the phone, and all pathology reports are faxed the same day they are diagnosed. We are available by phone if you need to discuss the diagnosis of a case with us.
Routine Formalin Fixed Tissue
POMPL provides biopsy kits upon request. Each biopsy kit consists of a formalin-filled plastic container, a history sheet and a business reply label addressed to our laboratory. We offer Priority Mail delivery through USPS. You can also request FedEx shipping prepaid labels.
Specimen Handling for Direct Immunofluorescence (DIF)
In order to help us process and diagnose your tissue samples, we offer the following guidelines.
- Specimens taken for DIF of bullous/desquamative lesions must be accompanied by another specimen for routine histopathology.
- Either two biopsies can be taken, or a single elliptical wedge can be procured and then hemisected.
- One specimen should go into formalin, the other into special DIF transport media supplied on request from our lab.
The diagnosis of bullous/desquamative lesions requires an assessment of where the epithelium is splitting. Clinically, obtaining these biopsies can be problematical due to the tendency for the epithelial layer to slough. It is best to seek a site in the anterior portion of the mouth and take care not to grasp the specimen with forceps. Eight-millimeter punch biopsies work quite well, and one should always biopsy the edge of the lesion to include both pathologic and normal-appearing tissues.
How does DIF Work?
Immunoglobulins from rabbits, goats or mice are used as reagents. These immunoglobulins are directed to antigens in the host tissue, and many of these antigens are immunoglobulins or autoantibodies (i.e. an antibody to an antibody). Many antigens are damaged by formalin fixation and tissue processing; therefore a special media is used and the sections are cut from frozen tissue samples.
The anti-human immunoglobulins are tagged with a fluorescent dye that can only be visualized with an ultraviolet light source (fluorescent) microscope.
How are results interpreted?
- Localization of fluorescent antibodies
- Basement membrane fibrinogen: lichen planus, lichenoid lesions
- Basement membrane C-3, IgG, IgM and/or IgA: mucous membrane pemphigoid
- Basement membrane IgM: lupus erythematosus
- Intercellular (desmosomal region) C-3, IgG, IgM and/or IgA: Pemphigus vulgaris
- Vascular wall C-3 and IgG: Erythema multiform
For the most part DIF is a useful adjunct for erosive diseases such as lichen planus, pemphigoid, pemphigus and erythema multiforme.
Due to limited storage times, please request DIF media only when you are ready to obtain a specimen for direct immunofluorescence. DIF tissue samples cannot be placed in formalin, since fixation damages the protein structure of many antigens and obfuscates the staining reaction. The transport media that we supply has a shelf life of about three months and can be refrigerated. It is advisable that media designated for direct immunofluorescent studies be refrigerated until use, but it can be transported at room temperature to the laboratory. For optimal results, please transport the specimen as soon as it is harvested in the designated container and send to the lab via FedEx.
Ordering
To order specimen packages, call 415.929.6560.
Please provide the requesting doctor's:
- First and last name
- Street address
- City, state and zip code
- Phone number in case of questions
Let us know how many you'd like and if you're new to our service.
Shipping Instructions
Free Return Shipping Instructions
- Pack the biopsy bottles in the same manner as you receive them.
- Wrap the biopsy bottle in a portion of paper towel and place it inside the plastic ziplock bag.
- Place the completed patient history sheet along with the sealed ziplock bag containing the biopsy bottle into our regular mailing can (for FedEx) or padded envelope (for U.S. Postal Service).
U. S. Postal Service:
Envelopes are addressed to us with your return address and include a prepaid postage stamp, priority mail sticker and a tracking sticker. Affix the larger tracking sticker onto the envelope containing the biopsy and place the smaller sticker in the patient's chart. A business reply label is provided on the padded envelope for your convenience. Just drop in any mailbox.
FedEx:
If you've had trouble with losses through the mail we offer return shipping by FedEx at no cost to you. Our packaging has been quality tested by the FedEx testing lab and is certified with FedEx #9001119506.
Just follow these instructions exactly:
- Call your local FedEx office to obtain FedEx Diagnostic Specimen Envelopes. You may request as many as you like. They will be delivered to you the next day. If you have any questions, call 1.800.GO.FEDEX (1.800.463.3339))
- Pack the biopsy bottles in the mailing cans as previously described.
- Place the mailing can(s) inside the FedEx Diagnostic Specimen Envelope and seal it according to the instructions on the envelope. You do not need additional absorbent material or outer packaging. The envelope can hold up to 10 cans.
- Affix the FedEx Billable Stamp Receipt provided with this mailing onto the envelope. Additional billable stamp receipts will be sent with new biopsy containers or upon request.
Biopsy Procurement Guidelines
The following guidelines are intended to guide medical professionals in properly preparing biopsies for sending to our lab.
Types of Biopsies
- Incisional biopsy: Sampling a portion of the lesion with a scalpel wedge incision or a punch.
- Excisional biopsy: Surgical removal of the entire lesion.
- Cytology smear for fungal stain ( must be fixed with alcohol and dried prior to sending)
Selecting a site
- For red, white and pigmented lesions, a biopsy can be taken anywhere within the lesional area.
- For bullous/erosive lesions, take an elliptical wedge incisional biopsy to include the lesion and a portion of normal adjacent tissue.
- Large masses: Take an incisional biopsy by obtaining a deep wedge, about a centimeter deep.
- Small masses: Excise the entire mass.
- Mucoceles: Include underlying glands to avoid recurrence.
- Gingival masses: Excise and perform thorough root planning.
- Ulcers: Small ones can be excised, Large ulcers should have an elliptical incision into the ulcer bed with inclusion of adjacent normal tissue.
Margins
Orient the specimen for anterior (or superior), posterior (or inferior), left margin, right margin. Place a short suture in the anterior (or superior) margin and a long suture in the right margin (or use one gut and one silk).
Do not use laser or cautery on epithelial lesions where dysplasia is expected. The artifactual changes can be severe and no diagnosis can be given. Use scalpel or punch, and after the tissue is removed, laser or cautery to the wound site can be applied for hemostasis.
Download the Biopsy Requisition Form.
In order to help us process and diagnose your tissue samples, we offer the following guidelines.
- Specimens taken for DIF of bullous/desquamative lesions must be accompanied by another specimen for routine histopathology.
- Either two biopsies can be taken, or a single elliptical wedge can be procured and then hemisected.
- One specimen goes into formalin, the other into special DIF transport media supplied on request from our lab.
The diagnosis of bullous/desquamative lesions requires an assessment of where the epithelium is splitting. Clinically, obtaining these biopsies can be problematical due to the tendency for the epithelial layer to slough. It is best to seek a site in the anterior portion of the mouth and take care not to grasp the specimen with forceps. Eight-millimeter punch biopsies work quite well, and one should always biopsy the edge of the lesion to include both pathologic and normal appearing tissues.
How does DIF work?
Immunoglobulins from rabbits, goats or mice are used as reagents. These immunoglobulins are directed to antigens in the host tissue and many of these antigens are immunoglobulins or autoantibodies (i.e. an antibody to an antibody). Many antigens are damaged by formalin fixation and tissue processing; therefore a special medium is used and the sections are cut from frozen tissue samples.
The anti-human immunoglobulins are tagged with a fluorescent dye that can only be visualized with an ultraviolet light source (fluorescent) microscope.
How are results interpreted?
- Localization of fluorescent antibodies
- Basement membrane fibrinogen: lichen planus, lichenoid lesions
- Basement membrane C-3, IgG, IgM and/or IgA: mucous membrane pemphigoid
- Basement membrane IgM: lupus erythematosus
- Intercellular (desmosomal region) C-3, IgG, IgM and/or IgA: Pemphigus vulgaris
- Vascular wall C-3 and IgG: Erythema multiform
For the most part DIF is a useful adjunct for erosive diseases such as lichen planus, pemphigoid, pemphigus and erythema multiforme.
The following guidelines are intended to guide medical professionals in properly preparing biopsies for sending to our lab
Types of biopsies
- Incisional biopsy: Sampling a portion of the lesion with a scalpel wedge incision or a punch.
- Excisional biopsy: Surgical removal of the entire lesion.
Selecting a site
- For red, white and pigmented lesions, a biopsy can be taken anywhere within the lesional area.
- For bullous/erosive lesions, take an elliptical wedge incisional biopsy to include the lesion and a portion of normal adjacent tissue.
- Large masses: Take an incisional biopsy by obtaining a deep wedge, about a centimeter deep.
- Small masses: Excise the entire mass.
- Mucoceles: Include underlying glands to avoid recurrence.
- Gingival masses: Excise and perform thorough root planning.
- Ulcers: Small ones can be excised, Large ulcers should have an elliptical incision into the ulcer bed with inclusion of adjacent normal tissue.
Margins
Orient the specimen for anterior (or superior), posterior (or inferior), left margin, right margin. Place a short suture in the anterior (or superior) margin and a long suture in the right margin (or use one gut and one silk).
Do not use laser or cautery on epithelial lesions where dysplasia is expected. The artifactual changes can be severe and no diagnosis can be given.Use scalpel or punch, and after the tissue is removed, laser or cautery to the wound site can be applied for hemostasis.
Free Return Shipping Instructions
- Pack the biopsy bottles in the same manner as you receive them.
- Wrap the biopsy bottle in a portion of paper towel and place it inside the plastic ziplock bag.
- Place the completed patient history sheet along with the sealed ziplock bag containing the biopsy bottle into our regular mailing can (for FedEx) or padded envelope (for U.S. Postal Service).
U. S. Postal Service:
A business reply label is provided on the padded envelope for your convenience. Just drop in any mailbox.
FedEx:
If you've had trouble with losses through the mail we offer return shipping by FedEx at no cost to you. Our packaging has been quality tested by the FedEx testing lab and is certified with FedEx #9001119506.
Just follow these instructions exactly:
- Call your local FedEx office to obtain FedEx Diagnostic Specimen Envelopes. You may request as many as you like. They will be delivered to you the next day. If you have any questions, call 1.800.GO.FEDEX (1.800.463.3339)
- Pack the biopsy bottles in the mailing cans as previously described.
- Place the mailing can(s) inside the FedEx Diagnostic Specimen Envelope and seal it according to the instructions on the envelope. You do not need additional absorbent material or outer packaging i.e. boxes, etc. The envelope can hold up to 10 cans.
- Affix the FedEx Billable Stamp Receipt provided with this mailing onto the envelope. Additional billable stamp receipts will be sent with new biopsy containers or upon request.
POMPL is not contracted with any insurance plans. We will bill your insurance as a courtesy. However, any unpaid balance remains your financial responsibility. The biopsy containers include a history sheet with an attached billing information sheet which you should tear off and give to your patient. This portion describes our service, how to send a payment and includes insurance information, if applicable, to be filled out.
In order to avoid billing problems or any misunderstandings, we would appreciate your cooperation in informing your patients of our separate fee for a single biopsy. When additional services are required (i.e. multiple biopsies, decalcification, special stains, and immunohistochemistry, additional fees will be applied.)
Our toll-free number for billing inquiries is 888.582.3397.
To best serve you and your patient, please take the time to completely fill out our history sheet. This enables us to give you a more definitive diagnosis. If radiographs or photos are pertinent and available, please enclose a copy if possible, or forward them under separate cover and they will be returned with the final report.
What If OSHA Pays a Visit?
OSHA has authority over two areas in the dental office: hazard communication (right-to-know laws) and infection control.
The hazard communication rule sets standards designed to ensure that products containing hazardous chemicals are properly handled by employees. The rule requires chemical manufacturers and importers to convey hazard information to employers through labels on containers and material safety data sheets (MSDSs). All employers must pass this information on to their employees.
In the area of infection control, OSHA is utilizing its general authority to regulate workplace safety by imposing basic infection control requirements on dental and other health care workers.
In order to enforce its workplace regulations, OSHA is authorized by statute to conduct workplace inspections.
From: The Journal of the Philadelphia County Dental Society, May/June 1989, Vol. 54, No. 6
Toxicity of Fixative Solution
OSHA Regulations on Toxic Materials in Dental Offices
- Material used: 10% buffered formalin
- Although formaldehyde is recognized as a toxic material, the solution sent to dental offices for use as a tissue fixative has been diluted and buffered with sodium phosphate.
- The solution provided in the biopsy kits is 10% formalin. Each bottle will be labeled as such to satisfy OSHA requirements.
- Each specimen bottle contains approximately 10 ml of this solution, and it is secured with a screw cap. As long as the cap is secure, the solution will not leak.
Material Safety Data Sheets
A copy of the Material Safety Data Sheet (MSDS) can be obtained from our supplier. Because of recent OSHA inspections of dental offices citing mishandling of hazardous chemicals, we are providing you with this sheet as a preventive measure to be posted or utilized as you see fit to follow OSHA guidelines.
Recommendations
- Specimen bottles should be kept tightly capped until just before usage.
- Tissue specimens should be placed in the specimen bottle and the cap secured. Care should be taken when collecting specimens to avoid contamination of the outside of the container. If contamination occurs, the container should be cleaned and disinfected as recommended by CDC and the ADA.
- Patient's name, date of biopsy and doctor's name should be marked on the specimen bottle as soon as it is recapped.
In the event of spillage, please refer to the sections on Health Hazards and Spill/Leak Procedures on the enclosed MSDS.
We thank you again for using our biopsy service. If you have any questions, please don't hesitate to contact us.
Business Associates Right to Privacy Declaration
As specified under the Health Insurance Portability and Accountability Act (HIPAA), Pacific Oral and Maxillofacial Pathology Laboratory (POMPL) herein provide a declaration of privacy to all of our contributing clinicians and surgeons.
POMPL receives biopsy specimens from your office/clinic along with demographic and historical data pertinent to the diagnosis.
Patient consent forms for submission of these materials to our laboratory are provided with biopsy mailer kits. This patient information is known only to key staff persons in our laboratory who are aware of the stipulations of law under the act.
Information Practices
No information regarding the patient or their diagnosis is transmitted to anyone other than yourself and our billing clearinghouse (Rand Medical Billing).
Copies of pathology reports are faxed to your office by our staff and must be handled in a confidential fashion with filing into appropriate storage systems that are not available to unauthorized scrutiny or entities outside your facility.
Other health professional agencies or individuals will be denied access to pathology findings without authorization by patient. Authorization forms will be provided upon request.
POMPL may request additional diagnostic material from other laboratories or imaging centers when it pertains to the diagnosis.
POMPL may request expert opinion from pathologists outside our establishment when the case is difficult and such consultations will benefit the healthcare of the patient.
If you have any questions about these policies, please contact:
Contact Person Regarding Complaints: Dr. Roy Eversole, 415.929.6560
The Oral and Maxillofacial Pathology Faculty at UOP are Medicare providers and are obliged to file claims to Medicare for all enrolled patients.
General dentists, or dental specialists other than surgeons should fill out form 855o, which is for these providers who are just going to order and refer and but will never bill Medicare.
Background
Bisphosphonates are non-metabolized analogs of pyrophosphate with a long period of retention in the bone (up to 10 years). Bisphosphonates can be chemically grouped into two main categories based on side chains.
The first category is the group containing nitrogen (which prevents metabolization; allowing them to accumulate with ongoing effects) and are considered more potent. Elendronate, risedronate, pamidronate, ibandronate and zoledronate are all members of this category. The medications inhibit farnesyl pyrophosphate synthesis and block the mevolanate pathway in osteoclasts.
The second group of medications is without the nitrogen side chain; and are considered less potent. This category includes etidronate, clodronate, and tiludronate.
Bisphosphonates induce osteoclast cell death by formation of cytotoxic metabolites of ATP-bisphosphonate analogs that interfere with intracellular metabolic enzymes. These medications are widely used among many medical disciplines with remarkable improvement in the overall quality of life in several conditions, including osteoporosis, Paget's disease, otosclerosis, immobilization due to malignancy-related hypercalcemia, fibrous dysplasia and osteolytic bone lesions of malignant myeloma and malignant diseases in which bone resorption is the main component of the disease.
Reports of Bisphosphonate-Related Osteonecrosis of the Jaw (BRONJ) were recognized as early as 2003. Currently, the American Academy of Oral & Maxillofacial Surgeons (AAOMS) define BRONJ as
- Current or previous treatment with a bisphosphonate;
- Exposed, necrotic bone in the maxillofacial region that has persisted for more than eight weeks; and
- No history of radiation therapy to the jaws.
BRONJ may be mistaken for several other conditions including alveolar osteitis, sinusitis, gingivitis/periodontitis, caries, periapical pathology and TMJ disorders.
Overall, the risk of developing BRONJ is estimated to be between 0.01% and 34%. Increased risk of developing BRONJ is increased with the potency of the medications and the duration of the therapy. Additionally, dentoalveolar surgery, extraction, dental implants, periapical, and other jaw surgeries are known local risk factors in causing the disease.
Precautions and Recommendations
The following must be kept in mind whenever clinicians see patients who are on bisphosphonates:
- Optimum OHI should be always emphasized, at all times, whether the patient is on or will be taking the medication. Patients who report history of diabetes, alcohol and tobacco usage taking corticosteroids or those receiving chemotherapeutic agents are considered at higher risk for developing BRONJ.
- Prior to treatment with IV bisphosphonates, a thorough oral examination with extraction of unsalvageable teeth, as well as the performance of any other invasive surgical procedures, should be completed.
- Discontinuation of oral bisphosphonates for a period of three months prior to and three months following elective invasive dental surgery may lower the risk of BRONJ. It is important, however, to remember that this medication is given for the presence of advanced metastatic carcinoma and multiple myeloma, among other serious conditions. Additionally, responses to discontinuing the medication vary with no concrete guarantees.
- When the clinician is planning to start the patient on bisphosphonates, it is highly preferred to delay dental treatments until optimal dental health is achieved. Again, this is done when a patient's systemic condition permits. Nevertheless, unsalvageable teeth and necessary surgical procedures should be completed. If the patient is already on IV-bisphosphonates and they are asymptomatic, invasive dentoalveolar surgeries or dental implants should be avoided. Non-restorable teeth may be treated by removal of the crown and endodontic treatment of the remaining roots.
- When the patient presents with convincing evidence of BRONJ, the necrotic bone and soft tissues should be debrided and all measures should be taken to achieve patient comfort and elimination of pain, with the understanding that there may be mixed results in response. Al elective surgical procedures must be delayed. Exposing uninvolved bone should be avoided at all times. Hyperbaric oxygen may or may not be effective. Discontinuation of the medication may potentially have a beneficial role in preventing BRONJ. However, clinicians must always weigh the benefits versus potential risk, providing that most patients receiving this class of medications have an advanced metastatic malignancy that requires long-term bisphosphonates therapy.
Detailed information on BRONJ can be found in the two position papers of the American Academy of Oral & Maxillofacial Pathology and the American Academy of Oral & Maxillofacial Surgery.
Immunohistochemical markers are monoclonal antibodies used to identify specific proteins in tissue sections. The antibody binds to the protein being assessed and a color reagent stains the protein, if in fact that protein is present in the tissue. The proteins that we search for indicate the differentiation of the tumor and help us to render a diagnosis. Identification of differentiation proteins is often required for tumors that cannot be readily classified on routine sections alone (e.g.: round cell tumors, spindle cell tumors).
We usually need to test for the presence of antibodies to the following proteins:
- Cytokeratins (a cocktail of keratin molecules of both low and high molecular weight: carcinomas and adenocarcinomas express these.
- Vimentin is an intermediate filament expressed in connective tissue tumors and melanomas
- LCA or leukocyte common antigen is found in leukemias and lymphomas
- CD20 is a protein found on B lymphocytes
- CD3 is a protein found on T lymphocytes
- CD34 is expressed in vascular tissue and certain subtypes of fibroblasts and is used to identify angiomas, angiosarcomas and specific types of fibroblastic neoplasms
- SMA or smooth muscle actin stains the actin intermediate filaments of contractile smooth muscle cells. Myofibroblastic and myoepithelial cell tumors express this marker
- Desmin is a muscle marker
- S-100 is an intermediate filament that stains neural cells as well as other cell types such as cartilage. It is employed for neural and granular cell tumors as well as melanocytic lesions
- HMB-45 stains some, but not all, melanomas
University of the Pacific, Arthur A. Dugoni School of Dentistry
155 Fifth Street
San Francisco, CA 94103
415.929.6560
Toll free: 866.958.3384
Fax: 415.929.6662
Director,, Darren P. Cox, DDS, MBA
Dr. Cox is Professor of Oral Pathology at the UOP, Arthur A. Dugoni School of Dentistry San Francisco, CA and director of the Pacific Oral Pathology Laboratory. He is a graduate of LSU School of Dentistry (’90). After a general practice residency at Loyola of Chicago Medical Center he practiced general dentistry in New Orleans for several years. Dr. Cox completed his residency in Oral, Head and Neck Pathology at Emory University Hospital, Atlanta, GA, in June 2000 and has been a board-certified oral and maxillofacial pathologist since 2001. Previous academic appointments were at the University of Pittsburgh School of Dental Medicine, where he also received a masters of business administration degree from the Katz Graduate School of Business in 2004, and at UCSF.
- The American Academy of Oral and Maxillofacial Pathology
- The American Academy of Oral and Maxillofacial Surgeons
- North American Society of Head and Neck Pathology
- United States and Canadian Academy of Pathology
- International Association of Oral Pathology
- The American Dental Association
- California Dental Society